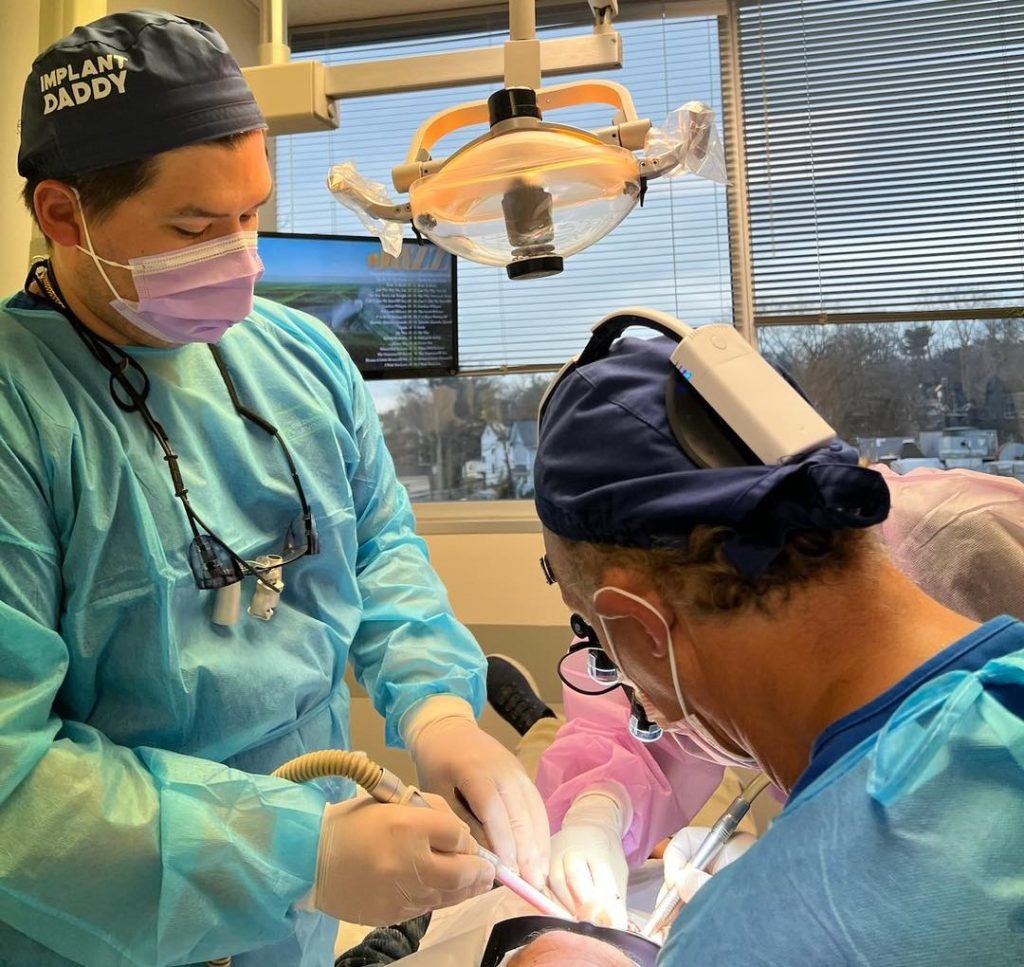
Placing a dental implant for the first time is not the same as reading about it, watching a video of it, or even practicing it on a typodont. The transition from theory to live surgery introduces variables that no textbook can fully prepare you for. Variables such as unexpected bleeding, bone density that does not match what the scan suggested, or a patient who flinches at the wrong moment. This is exactly why supervision during hands-on implant training is not just helpful. It is the single most important factor that determines whether a dentist walks away from a training program ready to treat patients safely or still guessing.
Many continuing education programs advertise hands-on experience, but the quality of that experience depends almost entirely on who is standing next to you while you work. This article examines why expert supervision is the variable that separates effective implant training from expensive observation, and what you should look for before enrolling in any hands-on implant surgical program.
The Learning Curve in Implant Dentistry Is Steeper Than Most Dentists Expect
There is a well-documented learning curve in implant surgery that affects even skilled general dentists. A 1997 study published in the Journal of Oral and Maxillofacial Surgery by Lambert, Morris, and Ochi found that implants placed by surgeons who had completed fewer than 50 cases failed at roughly twice the rate of those placed by more experienced surgeons. The most pronounced gap in failure rates appeared during the first nine cases, where inexperienced surgeons had a 5.9% failure rate compared to 2.4% for experienced ones. [1]
A 2019 retrospective study by Sonkar et al., published in the International Journal of Implant Dentistry, examined 1,449 implants placed by residents across three departments at Louisiana State University. Researchers grouped clinicians by training level and found that the most advanced group (third-year Periodontics and OMFS residents) achieved a 94.2% survival rate, compared to 88.6% for the beginner group (first-year Periodontics residents and Prosthodontics fellows). [2]
The takeaway is straightforward. The early cases are where dentists are most vulnerable to making errors, and these are precisely the cases where supervision matters most.
What Can Go Wrong Without Proper Oversight
Implant surgery is a procedure where millimeters matter. A drill angled a few degrees off or advanced a few millimeters too deep can result in complications that are difficult or impossible to reverse.
Nerve Injury
Inferior alveolar nerve (IAN) injury is one of the most serious risks in mandibular implant placement. A review by Juodzbalys, Wang, and Sabalys (2011) in the Journal of Oral and Maxillofacial Research reported that the incidence of IAN injuries during implant surgery ranges from 0% to 40% depending on the study and surgical context. Causes include direct drill penetration into the mandibular canal, thermal injury from excessive drilling speed, and implant intrusion that compresses the nerve. [3, 4]
When this happens during a supervised training session, the instructor can recognize warning signs in real time. A sudden change in resistance during drilling, unexpected bleeding, or a patient reporting an “electric shock” sensation are all cues that an experienced mentor will catch immediately. Without supervision, a less experienced clinician might continue the procedure past the point where the nerve has already been compromised.
Sinus Membrane Perforation
In the posterior maxilla, sinus membrane perforation during sinus augmentation procedures occurs in 22% to 50% of cases depending on technique and anatomy. While not always catastrophic, unrecognized or improperly managed perforations can lead to graft failure and infection. Supervised training gives the clinician a safety net: an experienced surgeon watching the procedure can identify a perforation the moment it happens and guide the trainee through the appropriate repair technique before the situation worsens. [5, 6]
Improper Implant Positioning
Placing an implant at the wrong angle, depth, or buccolingual position can compromise both the restorative outcome and long-term implant survival. These are not errors that show up immediately. They become apparent weeks or months later when the prosthetic does not seat properly, or when bone resorption begins around a poorly positioned fixture. A supervising instructor can correct positioning errors in real time, before the implant is fully seated, while a clinician working alone must live with the result.
How Does Supervision Actually Improve Training Outcomes?
Understanding that supervision matters is one thing. Understanding how it works at a practical level is what helps dentists choose the right program.
Real-Time Error Correction
The most obvious benefit of supervision is the ability to intervene before an error becomes a complication. In a supervised live surgery, the instructor is watching the same surgical field and can identify problems as they develop. This is fundamentally different from reviewing a case after the fact, where corrections are theoretical rather than practical.
Research on surgical training broadly supports the value of real-time feedback.
Building Pattern Recognition
Experienced implant surgeons have placed hundreds or thousands of implants. They have developed an intuitive sense for how bone should feel under the drill, what normal versus abnormal bleeding looks like, and when a case is progressing as expected versus heading toward a complication. This pattern recognition cannot be taught in a lecture. It transfers through close mentorship, where the instructor shares observations in real time and explains what subtle cues to watch for.
A scoping review by McGleenon and Morison, published in the British Dental Journal in 2021, examined methods for preparing dental students for independent practice in the UK and Ireland. The review found that safe practice of key operative skills before patient exposure, followed by supervised clinical practice, were essential elements for developing clinical competence. While the review focused on undergraduate dental education broadly rather than implant training specifically, its conclusions reinforce the principle that hands-on supervised experience is critical for building the clinical judgment needed for independent practice. [7, 8]
Confidence That Comes From Competence
There is an important distinction between confidence that comes from repetition and confidence that comes from supervised competence-building. Dentists who complete hands-on training under expert supervision report higher levels of readiness to treat patients independently, not because they have simply done the procedure many times, but because they have done it correctly under the guidance of someone who confirmed their technique was sound.
The AAID recognizes this distinction in its credentialing requirements. Candidates for Associate Fellow and Fellow credentials must complete 300 hours of education that includes both scientific coursework and clinical training, with at least one participatory (hands-on) course. The emphasis on structured, mentored clinical education reflects the understanding that unsupervised repetition alone does not produce competent implant surgeons. [9]
What Does Effective Supervision Look Like in an Implant Training Program?
Not all supervision is created equal. A program that advertises a 40:1 student-to-instructor ratio during live surgery is offering something fundamentally different from one with a 10:1 ratio, even if both technically involve “supervised” training.
Low Student-to-Instructor Ratios
Research on dental education consistently identifies low student-to-faculty ratio as where meaningful supervision occurs during practical sessions. At lower ratios, the instructor can devote adequate time to each student, observe their technique closely, and provide individualized feedback. Once ratios climb beyond that range, supervision becomes observation. The instructor may be present in the room, but they are not actively guiding each trainee through their case. [10]
Instructor Qualifications and Clinical Activity
The value of supervision is directly tied to the qualifications of the supervisor. An instructor who is board-certified, credentialed by organizations like the AAID, and actively placing implants in their own practice brings current, real-world expertise to the training environment. Dentists should ask about instructor credentials before enrolling in any program, and they should look for programs where the faculty includes surgeons with documented clinical experience in the specific procedures being taught.
Progressive Complexity With Guided Independence
The best supervised training programs do not simply let trainees watch a few cases and then hand them a handpiece. They use a progressive model where the clinician starts with simpler cases under close guidance and gradually takes on more complex procedures as the instructor confirms their readiness. This approach respects the learning curve documented in the research and ensures that trainees are not placed in situations that exceed their current skill level.
This progressive structure is what distinguishes programs like the AAID Maxicourse from short weekend workshops. A multi-session program with cumulative skill-building allows the instructor to track each participant’s development over time and adjust the level of supervision accordingly.
Why Lecture-Only and Model-Only Programs Fall Short
It would be unfair to say that lecture-based courses and simulation exercises have no value. They serve an important role in building foundational knowledge and introducing basic motor skills. But they do not replicate the conditions of live surgery, and they cannot substitute for supervised clinical experience.
A typodont does not bleed. A simulation model does not have variable bone density. A lecture cannot recreate the moment when a patient’s anatomy does not match the preoperative plan and the surgeon must make a judgment call in real time. These are the situations where supervision provides its greatest value, precisely because they are unpredictable and high-stakes.
The existing research on hands-on implant training consistently points to supervised live patient experience plus simulation as the training format that produces clinically prepared practitioners. Lectures build knowledge. Simulations build basic motor skills. Supervised surgery builds clinical judgment. [11, 12]
How to Evaluate Supervision Quality Before Enrolling
Dentists evaluating implant training programs should ask specific questions about the supervision structure before committing time and money.
Questions to Ask Any Program
Ask what the student-to-instructor ratio is during live surgical sessions, not just during lectures or lab work. Ask whether you will personally place implants under direct supervision or primarily observe. Ask about the credentials and active clinical experience of the instructors. Ask whether the program follows a progressive skill-building model or compresses everything into a single weekend.
Red Flags to Watch For
Programs that emphasize the number of CE credits over the quality of the clinical experience should raise concerns. Programs where the “hands-on” component consists entirely of typodont or model work with no live patient surgery under supervision are not preparing dentists for independent practice. Programs with class sizes that make meaningful one-on-one supervision impractical, regardless of how many instructors are listed on the brochure, should be evaluated critically.
What a Strong Program Looks Like
The strongest implant training programs combine didactic education with progressive, supervised clinical experience over multiple sessions. They maintain low student-to-instructor ratios during surgical sessions. Their faculty are credentialed, actively practicing, and available to guide trainees through each case from start to finish. They provide structured feedback, not just during the procedure, but in case review sessions where trainees can reflect on what went well and what needs improvement. [2, 13]
Frequently Asked Questions
Can I learn implant placement from online courses alone?
Online courses are valuable for building foundational knowledge in implant dentistry, including treatment planning, radiographic interpretation, and case selection. However, they cannot replace supervised hands-on training for developing the psychomotor skills and clinical judgment needed for live surgery. The most effective approach combines online or lecture-based education with in-person supervised clinical training.
How many supervised cases should I complete before placing implants independently?
While there is no universally agreed-upon number, research suggests that the steepest part of the learning curve occurs during the first 50 cases. The Lambert et al. study found that surgeons who had placed fewer than 50 implants had roughly double the failure rate of more experienced clinicians. Many structured training programs recommend completing a minimum number of supervised cases before transitioning to independent practice.
What complications are most likely during early implant cases?
The most common complications during early cases include improper implant positioning, inadequate primary stability due to errors in site preparation, inferior alveolar nerve injury during mandibular placement, and sinus membrane perforation during maxillary procedures. All of these complications are significantly easier to prevent or manage when an experienced instructor is supervising the case in real time.
Does the AAID require supervised training for credentialing?
The AAID requires 300 hours of education for Associate Fellow credentialing, divided between scientific coursework and clinical training. At least one course must be participatory, meaning hands-on. Candidates must also submit documented case reports demonstrating clinical competence. While the AAID does not mandate a specific number of supervised surgical hours, the credentialing process is designed to ensure that candidates have meaningful clinical experience beyond lecture-based education.
How do I know if a program’s supervision is actually hands-on?
Ask whether you will personally perform surgical procedures during the program or primarily observe. Ask about the student-to-instructor ratio during the surgical component specifically, not the overall program. Ask whether instructors provide real-time guidance during your cases or only review them afterward. Programs that are transparent about these details are typically the ones that deliver genuine supervised training.
References
1. https://pubmed.ncbi.nlm.nih.gov/9393421/
2. https://pmc.ncbi.nlm.nih.gov/articles/PMC6687780/
3. https://pmc.ncbi.nlm.nih.gov/articles/PMC3886063/
4. https://pmc.ncbi.nlm.nih.gov/articles/PMC4306320/
5. https://pmc.ncbi.nlm.nih.gov/articles/PMC10932102/
6. https://pmc.ncbi.nlm.nih.gov/articles/PMC11242322/
7. https://pmc.ncbi.nlm.nih.gov/articles/PMC7791324/
8. https://pmc.ncbi.nlm.nih.gov/articles/PMC10586436/
9. https://www.aaid.com/credentialing-faq
10. https://www.estheticadentalchandigarh.com/what-is-the-student-to-faculty-ratio-for-hands-on-training/
11. https://pmc.ncbi.nlm.nih.gov/articles/PMC7246576/
12. https://pmc.ncbi.nlm.nih.gov/articles/PMC12116900/
13. https://pmc.ncbi.nlm.nih.gov/articles/PMC11916869/